Daniela Barros, post graduate student of the Surgical Clinic Program at Ribeirão Preto Medical School, University of São Paulo (FMRP-USP), Ribeirão Preto, SP, Brasil.
 Papillary thyroid carcinoma (PTC) is the most common thyroid cancer. Follicular thyroid lesions with nuclear characteristics of papillary carcinoma are classified as an infiltrative follicular variant of papillary thyroid carcinoma (IFVPTC) and follicular variant of papillary thyroid carcinoma (FVPTC) with tumor capsular invasion (IEFVPTC). (JUNG, C.K., et al.; ROSAI, J., CARCANGIU, M.L. and DeLELLIS, R.A.; LUI, J., et al.)
Papillary thyroid carcinoma (PTC) is the most common thyroid cancer. Follicular thyroid lesions with nuclear characteristics of papillary carcinoma are classified as an infiltrative follicular variant of papillary thyroid carcinoma (IFVPTC) and follicular variant of papillary thyroid carcinoma (FVPTC) with tumor capsular invasion (IEFVPTC). (JUNG, C.K., et al.; ROSAI, J., CARCANGIU, M.L. and DeLELLIS, R.A.; LUI, J., et al.)
Although FVPTC is generally associated with a better prognosis than classic PTC(SHI, X., et al.), there are still questions as to the behavior of its histological subtypes. Recently, a group of experts compared patients with encapsulated/well demarcated FVPTC with tumor capsular invasion (IEFVPTC) against those without vascular and/or tumor capsule invasion (non-invasive, NI); they reported that the non-invasive tumor had a distinct behavior with a very low risk of progression, proposing the name non-invasive follicular thyroid neoplasms with papillary-like nuclear features, or NIFTP. (NIKIFOROV, Y.E., et al.)
Based on these findings, the World Health Organization (WHO) added NIFTP to their classification list of endocrine tumors, with diagnosis based on very specific histopathological criteria such as well-defined lesion demarcation, absence of capsular of vascular infiltration, and the presence of atypical nuclear features similar to those in PTC. (LLOYD, R.V., et al.,) Thus, only a very specific subset of non-invasive encapsulated tumors can now be reclassified as NIFTP.
In a multicentric study conducted by a team from the Universidade Estadual Paulista (Unesp), Botucatu (Brazil), under the coordination of Bárbara Parente Coelho, in collaboration with researchers from the Universidade do Porto, in Portugal, it was evaluated whether the computerized image analysis would be able to identify nuclear differences between these three tumor subtypes.
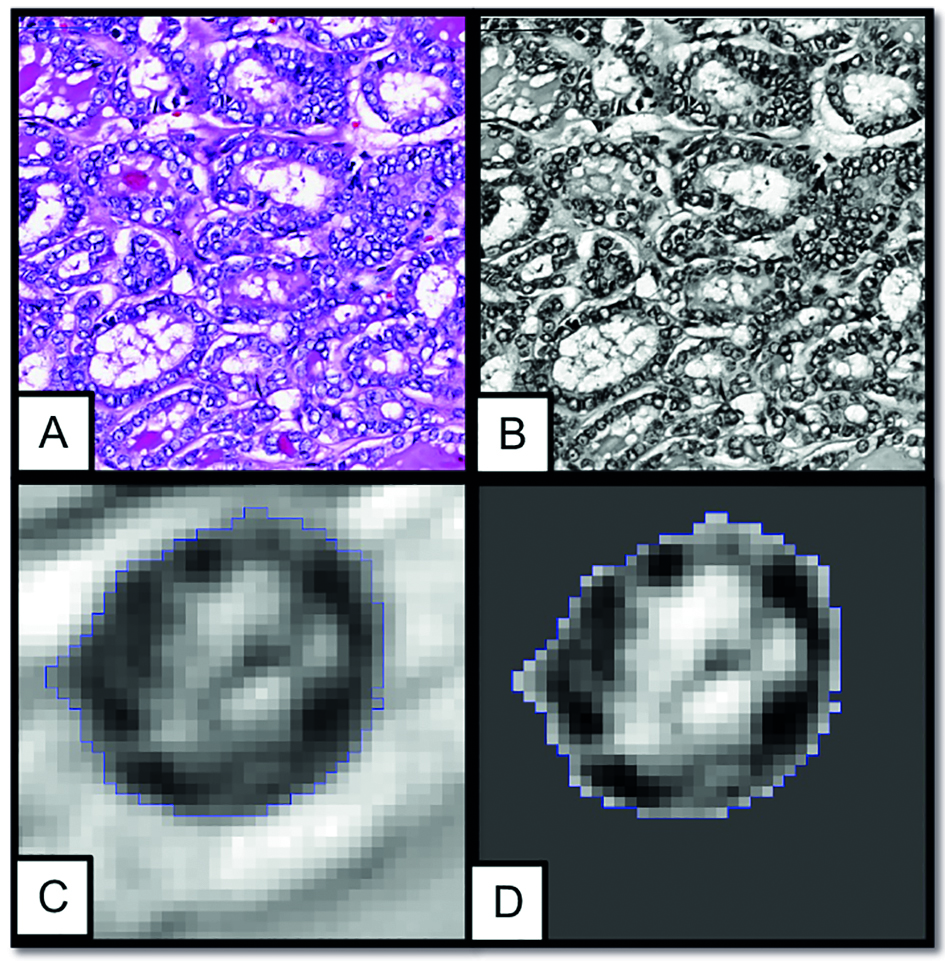
Slide photo exemplifying the morphometric analysis of the histological material of a follicular variant of papillary carcinoma (FVPTC) under analysis by Image J program. The program transforms the millions of tones of the captured color images into 256 tones of grey (grey-scale, 16-bits), considerably reducing the number of tones in the nuclei images, allowing a much clearer evaluation of chromatin compaction level and better homogeneity between samples despite differences in color A: color photo; B: grey-scale photo; C and D: selected nucleus.
Based on this research, the article “Follicular Lesions with Papillary Nuclear Characteristics: Differences in Chromatin Detected by Computerized Image Analysis” was published in Archives of Endocrinology and Metabolism (vol. 64, no. 5).
Slides with histological material from 15 cases of NIFTP and 33 cases of FVPTC subtypes (22 IEFVPTC, and 11 IFVPTC) were analyzed using the Image J image processing program. Tumor cells were compared for both nuclear morphometry and chromatin textural characteristics. Nuclei from NIFTP and IFVPTC tumors differed in terms of chromatin textural features (grey intensity): mean (92.37 ± 21.01 vs 72.99 ± 14.73, p = 0.02), median (84.93 ± 21.17 vs 65.18 ± 17.08, p = 0.02), standard deviation (47.77 ± 9.55 vs 39.39 ± 7.18; p = 0.02), and coefficient of variation of standard deviation (19.96 ± 4.01 vs 24.75 ± 3.31; p = 0.003).
Significant differences were observed between NIFTP and IFVPTC. Overall, the differential between infiltrative (IFVPTC) and encapsulated FVPTC depends on evaluating a series of both qualitative and quantitative histological parameters. Differentiation between the encapsulated lesions (NIFTP and IEFVPTC), in turn, would be based on more complex morphological criteria, i.e., the presence of vascular and capsular invasion, quantification of mitotic activity, the presence of papillary structures, and solid/trabecular/insular growth pattern, as well as using nuclear scores. (NIKIFOROV, Y.E., et al.)
However, as the researchers explain, all this analysis requires highly specialized training and meticulous evaluation, as well as the adequate supply and preparation of histological material. In this sense, tools that can help in the diagnostic process would be very welcome.
In conclusion, the authors observed that a computerized image analysis tool detected nuclear textural differences between NIFTP and IFVPTC, but not between NIFTP and IEFVPTC. Therefore, optimization of this technique, with the integration of additional morphological, genetic or histopathological parameters, could represent a useful complementarydiagnostic tool for evaluating follicular patterned lesions with papillary-like nuclear characteristics.
References
JUNG, C.K. et al. The increase in thyroid cancer incidence during the last four decades is accompanied by a high frequency of BRAF mutations and a sharp increase in RAS mutations. J Clin Endocrinol Metab [online]. 2014, vol. 99, no. 2, pp. E276-E285. [viewed 11 November 2020]. https://doi.org/10.1210/jc.2013-2503. Available from: https://academic.oup.com/jcem/article/99/2/E276/2537161
LIU, J. et al. Follicular variant of papillary thyroid carcinoma: a clinicopathologic study of a problematic entity. Cancer [online]. 2006, vol. 107, no. 6, pp. 1255-1264 [viewed 11 November 2020]. https://doi.org/10.1002/cncr.22138. Available from: https://acsjournals.onlinelibrary.wiley.com/doi/full/10.1002/cncr.22138
Lloyd R.V. et al. WHO Classification of Tumors of Endocrine Organs. 4th ed. Lyon: IARC Press; 2017.
NIKIFOROV, Y.E. et al. Nomenclature Revision for Encapsulated Follicular Variant of Papillary Thyroid Carcinoma: A Paradigm Shift to Reduce Overtreatment of Indolent Tumors. JAMA Oncol [online]. 2016, vol. 2, no. 8, pp. 1023-1029 [viewed 11 November 2020]. https://doi.org/10.1001/jamaoncol.2016.0386. Available from: https://jamanetwork.com/journals/jamaoncology/fullarticle/2513250
ROSAI, J. et al. Atlas of Tumor Pathology. Washington, DC: Armed Forces Institute of Pathology. The Journal of Pathology [online]. 1993, vol. 171, no. 3, pp. 247-248 [viewed 11 November 2020]. https://doi.org/10.1002/path.1711710319. Available from: https://onlinelibrary.wiley.com/doi/10.1002/path.1711710319
SHI, X. et al. Differential Clinicopathological Risk and Prognosis of Major Papillary Thyroid Cancer Variants. J Clin Endocrinol Metab. [online]. 2016, vol. 101, no. 1, pp. 264-274 [viewed 11 November 2020]. https://doi.org/10.1210/jc.2015-2917. Available from: https://academic.oup.com/jcem/article/101/1/264/2806832
To read the article, acess
COELHO, B.P. et al. Follicular lesions with papillary nuclear characteristics: differences in chromatin detected by computerized image analysis. Arch Endocrinol Metab. [online]. 2020, vol. 64, no. 5, pp. 630-635 [viewed 11 November 2020]. https://doi.org/10.20945/2359-3997000000282. Available from: http://ref.scielo.org/5s7qt3
External links
Bárbara Parente Coelho: https://orcid.org/0000-0002-1440-2196
Archives of Endocrinology and Metabolism – AEM: https://www.scielo.br/aem
Como citar este post [ISO 690/2010]:

















Recent Comments