Daniela Barros, special student at the Department of Public Health, Ribeirão Preto Medical School, University of São Paulo (FMRP-USP). Ribeirão Preto, SP, Brazil.
 The article Supplements for bone health published in the Archives of Endocrinology and Metabolism, vol. 70, special issue 1 (da SILVA, T.D.B., et al., 2026) concludes that supplementation with calcium and vitamin D can reduce bone loss and fracture risk in selected populations, particularly older adults, institutionalized individuals, and those with documented deficiencies, while evidence supporting routine supplementation with vitamin K, magnesium, and phosphorus remains limited, heterogeneous, or context dependent.
The article Supplements for bone health published in the Archives of Endocrinology and Metabolism, vol. 70, special issue 1 (da SILVA, T.D.B., et al., 2026) concludes that supplementation with calcium and vitamin D can reduce bone loss and fracture risk in selected populations, particularly older adults, institutionalized individuals, and those with documented deficiencies, while evidence supporting routine supplementation with vitamin K, magnesium, and phosphorus remains limited, heterogeneous, or context dependent.
The review was conducted by researchers from the Division of Endocrinology at the Federal University of São Paulo (UNIFESP), led by Dr. Tiago Donizeti Bertolacini da Silva, and published as part of the special issue Voices of Endocrinology: contemporary insights in endocrine and metabolic disorders.
The growing use of dietary supplements for bone health, often driven by physiological plausibility rather than robust clinical outcomes, provided the main motivation for this review. While calcium and vitamin D are firmly established as key regulators of bone metabolism, the clinical relevance of supplementing other micronutrients has remained uncertain. At the same time, increasing reports of adverse events associated with excessive or inappropriate supplementation have raised concerns about indiscriminate use. Against this backdrop, the authors sought to critically reassess the balance between potential benefits and risks across commonly used bone-related supplements.
Bone health is shaped by a complex interaction of genetic, hormonal, and environmental factors, with nutrition playing a central role throughout life. Calcium and vitamin D are fundamental to skeletal integrity and mineral homeostasis, whereas vitamin K, magnesium, and phosphorus contribute through distinct biochemical and cellular mechanisms. Despite this physiological importance, clinical evidence supporting supplementation varies widely among these nutrients. The review also places particular emphasis on the Brazilian context, where population-based studies consistently show inadequate dietary intake of calcium and vitamin D across different age groups, potentially contributing to the high prevalence of osteoporosis and fragility fractures observed in the country.
Methodologically, the review synthesized data from meta-analyses, systematic reviews, randomized clinical trials, and observational studies addressing five key micronutrients involved in bone metabolism: calcium, vitamin D, vitamin K, magnesium, and phosphorus. The authors examined physiological mechanisms, dietary reference values, national intake patterns, and clinical outcomes related to supplementation, with particular attention to fracture risk, bone mineral density, and adverse events.
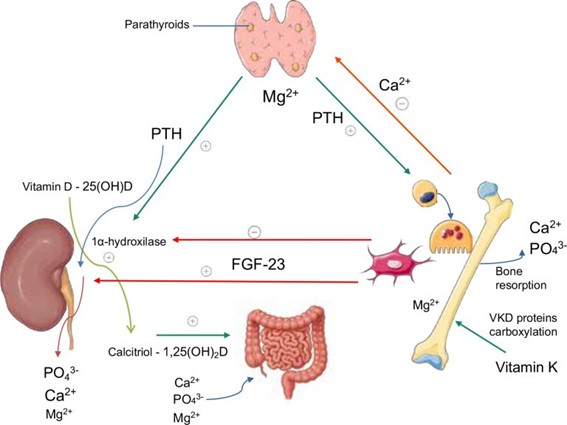
Image: from the article.
Figure 1. Interactions among the main regulators of mineral metabolism.
Regarding calcium and vitamin D, meta-analyses show modest reductions in fracture risk and bone loss, particularly when both are combined and targeted to older or deficient individuals. However, large trials, including the Women’s Health Initiative, indicate that benefits are largely confined to specific subgroups, with no significant fracture reduction in the general population and a reported increase in nephrolithiasis in some studies.
Regarding vitamin K, observational studies associate low intake and circulating levels with reduced bone mineral density and higher fracture risk, particularly hip fractures. However, randomized trials show inconsistent results, with potential benefits mainly observed in osteoporotic populations, long-term studies, or Japanese cohorts, providing insufficient evidence to support routine supplementation in the general population.
Magnesium is recognized as a critical cofactor in bone matrix synthesis, vitamin D activation, and calcium homeostasis. The review underscores that both deficiency and excess magnesium can adversely affect bone health.
Phosphorus, although essential for skeletal mineralization, is generally abundant in the diet. The authors emphasize that supplementation is rarely indicated in individuals with normal renal function and adequate intake, and that excessive phosphorus consumption may disrupt mineral metabolism, particularly in patients with chronic kidney disease.
In discussing the broader implications of the evidence, the authors highlight important limitations in the current literature. Many trials were not designed with fracture outcomes as primary endpoints, follow-up durations were often insufficient, and substantial heterogeneity exists regarding supplement formulations, dosages, and baseline nutritional status. These factors limit the ability to draw definitive conclusions, especially for micronutrients other than calcium and vitamin D (ROJAS-FERNANDEZ, C.H., et al., 2012; MYUNG, S.K., et al., 2021).
The review also draws attention to safety concerns. Calcium supplementation, particularly at high doses or when used without vitamin D, has been associated in some studies with gastrointestinal intolerance, nephrolithiasis, and a potential increase in cardiovascular risk, although findings remain inconsistent and methodologically constrained (BOLLAND, M.J., et al., 2010; BOLLAND, M.J. et al., 2011). These observations reinforce the need for caution and individualized decision-making.
In conclusion, the authors argue that bone health strategies should prioritize dietary sources of micronutrients and reserve supplementation for individuals with documented deficiencies, increased fracture risk, or specific clinical indications. An individualized, evidence-informed approach is essential to maximize benefits while minimizing potential harm. The review calls for future well-designed randomized trials with fracture outcomes, longer follow-up, and better characterization of at-risk populations, particularly for vitamin K and magnesium, as supplement use continues to expand worldwide.
To read the article, access
SILVA, T.D.B. Supplements for bone health. Arch Endocrinol Metab. [online]. 2026, vol. 70 (special issue), no. 1, pp. 1-30. [viewed 11 February 2026]. https://doi.org/10.20945/2359-4292-2025-0374. Available from: https://www.scielo.br/j/aem/a/nKFhWSfQRdphz76TTLB95kz/
References
BOLLAND, M.J., et al. Calcium supplements with or without vitamin D and risk of cardiovascular events: reanalysis of the Women’s Health Initiative limited access dataset and meta- analysis. BMJ [online]. 2011, vol. 342, pp. d2040. [viewed 11 February 2026]. https://doi.org/10.1136/bmj.d2040. Available from: https://pubmed.ncbi.nlm.nih.gov/21505219/
BOLLAND, M.J., et al. Effect of calcium supplements on risk of myocardial infarction and cardiovascular events: meta-analysis. BMJ [online]. 2010, vol. 341, pp. c3691. [viewed 11 February 2026]. https://doi.org/10.1136/bmj.c3691. Available from: https://pubmed.ncbi.nlm.nih.gov/20671013
MYUNG, S.K., et al. Calcium Supplements and Risk of Cardiovascular Disease: A Meta-Analysis of Clinical Trials. Nutrients [online]. 2021, vol. 13, no. 2, pp. 368. [viewed 11 February 2026]. https://doi.org/10.3390/nu13020368. Available from: https://pubmed.ncbi.nlm.nih.gov/33530332/
ROJAS-FERNANDEZ, C.H., et al. Assessing the potential adverse consequences of supplemental calcium on cardiovascular outcomes: should we change our approach to bone health? Ann Pharmacother [online]. 2012, vol. 46, no. 5, pp. 696-702. [viewed 11 February 2026]. https://doi.org/10.1345/aph.1q627. Available from: https://pubmed.ncbi.nlm.nih.gov/22570431/
External links
Archives of Endocrinology and Metabolism – AEM
Como citar este post [ISO 690/2010]:
















Recent Comments